"The Thymus Has Been Overlooked for Decades"
A Butterfly-Shaped Organ That Science Got Wrong
For generations, medical students were taught a single, confident fact about the thymus gland: it stops mattering after puberty. The organ shrinks as we age. It produces fewer T-cells. By adulthood, doctors assumed, it had effectively retired from active duty.
Two studies published simultaneously in Nature on March 18, 2026, challenge this assumption with the largest body of evidence ever assembled on the subject.
"The thymus has been overlooked for decades and may be a missing piece in explaining why people age differently, and why cancer treatments fail in some patients," said Hugo Aerts, PhD, corresponding author on both papers and director of the Artificial Intelligence in Medicine (AIM) Program at Mass General Brigham. "Our findings suggest thymic health deserves much more attention and may open new avenues for understanding how to protect the immune system as we age."
That quote from one of Harvard's most senior AI medicine researchers, published across the Harvard Gazette and the official Mass General Brigham press release, is the headline beneath the headline. Scientists are not saying the thymus might be important. They are saying medicine got it wrong, and they now have data from 27,000 people to demonstrate exactly how wrong.
What the Thymus Actually Does: The Body's Immune Training Camp
Why T-Cells Are the Soldiers Your Body Cannot Fight Without
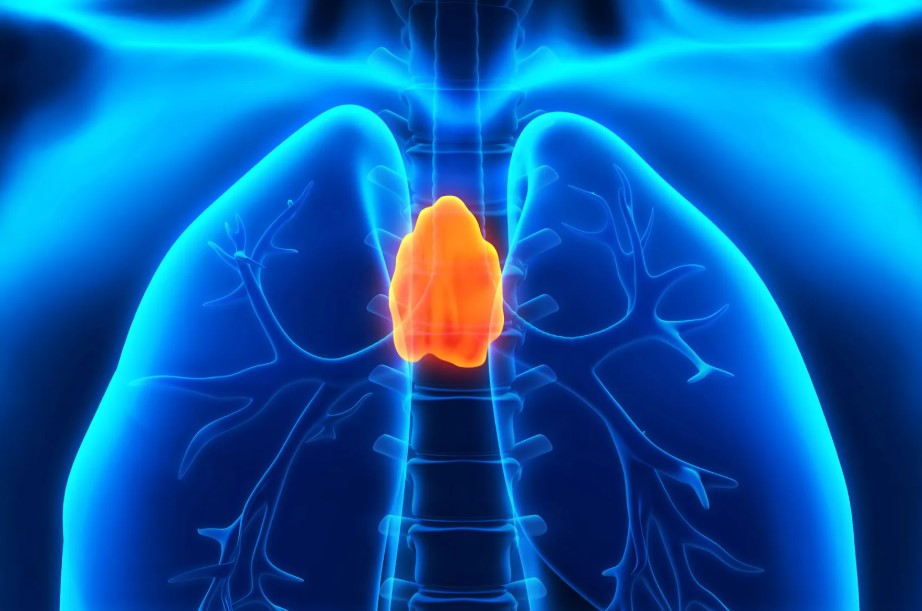
The thymus is a small, butterfly-shaped gland sitting in the upper chest, just behind the breastbone and in front of the heart. Its primary biological function is to take immature immune cells produced in bone marrow and train them into functional T-cells, the specialised white blood cells that identify and destroy infected cells, cancer cells, and foreign pathogens.
This training process is extraordinarily precise. A T-cell that attacks healthy tissue is a liability. A T-cell that fails to recognise a cancer cell is a missed opportunity. The thymus eliminates both errors through a selection process that refines the immune system's recognition capability before T-cells are released into circulation.
The problem, as doctors have historically understood it, is that the thymus undergoes "thymic involution," a gradual shrinkage and decline in output that accelerates after puberty and continues through adulthood. By middle age, the thymus is largely fatty tissue in most people. Or so the thinking went.
What the Mass General Brigham research found is that this involution is not uniform and not inevitable at the same rate across all people. The character and speed of thymic decline vary widely across the population, and that variation has direct, measurable consequences for how long you live and how well your body fights disease.
The Four Numbers That Change Everything
What a Healthy Thymic Score Means in Practice
People with high thymic health scores had about a 50% lower risk of death, 63% lower risk of cardiovascular death, and 36% lower risk of developing lung cancer compared to those with low thymic health. These associations remained significant after adjusting for age and other health factors.
These are not marginal statistical differences. They are large, clinically meaningful associations that held up even after researchers adjusted for age, sex, smoking status, and existing health conditions. That last point matters. The thymus benefit was not simply a proxy for being young or not smoking. Even controlling for those factors, thymic health independently predicted survival and disease outcomes.
In the second study of 1,200 patients receiving immunotherapy, those with a robust thymus had a 37% lower risk of their cancer getting worse and a 44% lower risk of death.
The immunotherapy finding is especially significant. Immunotherapy, the fastest-growing class of cancer treatments in the world, works by activating the patient's own immune system to attack cancer cells. Its effectiveness is entirely dependent on the strength and quality of the patient's immune response. The finding that thymic health directly predicts immunotherapy response means that this one organ may explain a substantial portion of why the same treatment produces dramatically different outcomes in different patients.
How AI Made This Discovery Possible
27,000 Scans, One Deep Learning Framework
The research team developed a deep learning framework to quantify thymic health from routine radiographic images and evaluated its association with longevity and risk of major age-associated diseases in two large prospective cohorts: the National Lung Screening Trial (n = 25,031) and the Framingham Heart Study (n = 2,581).
The National Lung Screening Trial followed participants for 12 years. The Framingham Heart Study is one of the longest-running cardiovascular research programmes in medical history. By applying AI to the CT scans already collected by these studies, the researchers were able to extract thymic health data that no prior study had ever analysed at this scale.
The AI model assessed the size, shape, and tissue composition of the thymus in each scan, generating a thymic health score that correlated with long-term health outcomes across a 12-year follow-up period. This is the methodological achievement that makes the findings significant: not just the result, but the scalability of the measurement tool.
Routine CT scans are already performed on millions of patients every year for other reasons, from cancer screening to cardiac assessment. An AI overlay capable of extracting thymic health scores from those existing scans would require no new procedures, no additional imaging costs, and no patient inconvenience.
What Damages Your Thymus: The Three Lifestyle Factors
"Chronic Inflammation, Smoking, and High Body Weight"
The researchers' analysis found that chronic inflammation, smoking, and high body weight were associated with poorer thymic health, suggesting that lifestyle and systemic inflammation may influence immune resilience across the lifespan.
This finding transforms the thymus from a passive bystander in ageing into an active target for health intervention. If lifestyle choices damage the thymus, then lifestyle changes could theoretically protect or even partially restore its function.
Three specific factors deserve attention:
Smoking: Tobacco smoke is an established immunosuppressant. The association between smoking and thymic decline in this dataset adds a specific mechanistic pathway to what was previously understood as a general immune suppression effect.
High body weight: Adipose tissue, particularly visceral fat, produces inflammatory cytokines that chronically activate the immune system at low levels. This background inflammation appears to accelerate thymic involution beyond the age-related rate.
Chronic inflammation: Whether from metabolic syndrome, autoimmune conditions, or persistent infections, systemic inflammation consistently predicted poorer thymic health scores in the dataset.
The researchers propose looking at whether changing lifestyle factors might improve thymic function, while noting that the current studies did not directly test whether modifying those factors can reverse thymic decline.
What This Means for You Right Now: The Honest Assessment
"The Imaging Method Is Not Yet Ready for Routine Clinical Use"
Before this finding changes how you think about your next medical appointment, three important caveats apply.
Because this was an observational study, the findings do not establish causality, and it remains unclear whether reduced thymic health drives disease risk or reflects underlying health decline. Additionally, the study populations were predominantly White and included specific cohorts, such as heavy smokers in the NLST, which may limit generalisability to broader populations.
In plain language: the study shows a powerful correlation between thymic health and survival. It does not yet prove that improving thymic health will improve survival. The direction of causality, whether a healthy thymus causes better health outcomes or whether healthier people happen to have healthier thymuses, has not been definitively established.
The imaging method is not yet ready for routine clinical use. There is no validated clinical pathway through which your doctor can order a thymic health score alongside your standard blood panel. That infrastructure does not yet exist.
What does exist is a strong scientific signal that the medical community has been undervaluing a significant predictor of adult health for decades, and that signal is now published in Nature, sourced from 27,000 participants, and being replicated and extended by the same research team.
What Comes Next in Thymus Research
"Thymic Health Deserves Much More Attention"
The Mass General Brigham team is currently running two active follow-on studies. The first examines whether unintended radiation exposure to the thymus in lung cancer patients affects their treatment outcomes, directly relevant to radiotherapy planning for chest tumours. The second investigates whether lifestyle interventions or anti-inflammatory treatments can measurably improve thymic function in adults.
The researchers suggest the thymus might provide a new target for personalising disease prevention and cancer treatments, potentially allowing physicians to better assess disease risk and guide treatment decisions based on thymic health scores derived from routine imaging.
If that research confirms that thymic health is modifiable through lifestyle or pharmacological intervention, the clinical implications are substantial. It would mean that a measurable biomarker, obtainable from an existing imaging type, could be used to personalise preventive health recommendations, stratify cancer immunotherapy candidates, and track immune resilience over time.
Conclusion: Thymus Gland Longevity Research Has Permanently Changed What We Know About Ageing
The thymus gland longevity study published in Nature on March 18, 2026, is one of the most consequential pieces of immunology research in years. It does not merely add a data point to an existing body of knowledge. It overturns a decades-long consensus that the thymus is irrelevant in adult health.
"Improving our understanding and monitoring of thymic health could eventually help physicians better assess disease risk and guide treatment decisions," said Aerts.
For now, the most evidence-based takeaway is specific and actionable: the three lifestyle factors most consistently associated with poor thymic health are smoking, excess body weight, and chronic inflammation. All three are modifiable. None of the interventions required to address them are novel or expensive.
You may not be able to order a thymic health score at your next check-up. But the evidence is now strong enough to say that avoiding the habits which shrink and damage your thymus is not just good general health advice. It is, specifically, advice about preserving the organ that trains your immune system to keep you alive longer.
That organ is small. It is butterfly-shaped. And medicine largely ignored it for 50 years. It is unlikely to be ignored much longer.




Comments (0)
Leave a Comment
No comments yet
Be the first to comment